
In most of the peripheral lung fields of a normal, healthy patient, vesicular sounds should be soft and lower in pitch with a longer inspiration and a shorter expiration with no pause between. Moving past the segmental bronchi, the sounds become more reduced because the chest wall, muscles and lung tissues muffle the sounds. They can be described as “hollow” or “tunnel like” and there is no pause between inspiration and expiration. Bronchial sounds are loud and can be high or low pitched. Posterialy, bronchial sounds can be heard on either side of the spinal column from the third rib to the sixth rib. Air moves quickly through these airways and the sounds should be easily identifiable.Īt the trachea the airflow sounds high pitched and there is a noteworthy pause at the end of inspiration followed by expiratory flow that is about double the length of the inspiratory time.Īs you move to either side of the sternum, anteriorly, bronchial breath sounds can be heard between the second rib (intercostal space) and the fourth rib. Sounds heard near the large airways will be loud and somewhat harsh. Normal breath sounds can be heard over the large airways such as the trachea and bronchus and bilaterally throughout the lung fields. The NBRC breaks down breath sounds into Normal “Vesicular” and Abnormal “Adventitious” sounds. When it comes to auscultation, just like everything else in respiratory school, knowing what is normal is the best way to recognize when something is abnormal. That said, we cannot stop medical providers who came before us from using obsolete terminology, but we can be sure we don’t confuse ourselves when we sit for our boards. and yet, many of these words no longer have a place on your board exams so they aren’t taught in respiratory class. You know, THESE words: rales, rhonchus, crepitations, wheezes, sonorous exhalations, crackles, etc. In clinical rotations you hear ALL the words that have ever been used to describe lung sounds. It is no wonder that this skill can be such a head scratcher for students. Part of the puzzlement comes from the confusion about terminology over the years. Understanding what each sound is, how to categorize it, and what to do about it is such a critical skill in our field and yet it can all be very confusing for students. Further studies are indicated to validate the accuracy and potential clinical benefit of auscultation in detecting pulmonary abnormalities in COVID-19 infection.Auscultating, or listening to, the lung sounds of pulmonary patients is going to be something a respiratory therapist does at least 20 times a day if not much more. 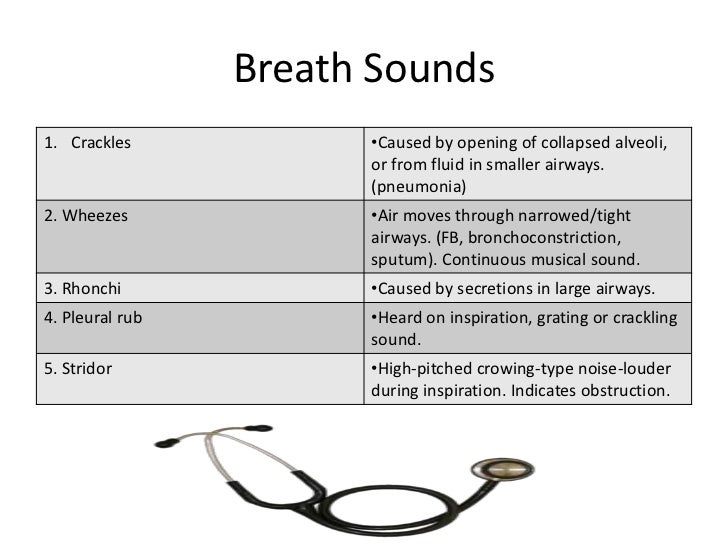
Such evidence suggests that electronic auscultation is useful to aid diagnosis and timely management of the disease. Conclusions: The abnormal breath sounds in COVID-19 pneumonia had some consistent distributive characteristics and to some extent correlated with the radiologic features. The presence of fine and coarse crackles detected 33/39 patients with ground-glass opacities (sensitivity 84.6% and specificity 12.5%) and 8/9 patients with consolidation (sensitivity 88.9% and specificity 15.2%), while the presence of Velcro crackles identified 16/39 patients with ground-glass opacities (sensitivity 41% and specificity 81.3%). Most cases had normal breath sounds in upper lungs, but the proportions of abnormal breath sounds increased in the basal fields where Velcro crackles were more commonly identified at the posterior chest. High-quality auscultation recordings (98.8%) were obtained, and coarse breath sounds, wheezes, coarse crackles, fine crackles, and Velcro crackles were identified. Most cases had bilateral lesions (96.4%) such as multiple ground-glass opacities (69.1%) and fibrous stripes (21.8%). The most common symptoms were cough (73.7%) during auscultation. Results: Fifty-seven patients with average age of 60.6 years were enrolled. 
Standard auscultation with an electronic stethoscope was performed and electronic recordings of breath sounds were analyzed. 
Methods: This cross-sectional, observational study was conducted among patients with laboratory-confirmed COVID-19 at Wuhan Red-Cross Hospital during the period from January 27, 2020, to February 12, 2020. Objectives: The aim of this study was to explore the features and clinical significance of pulmonary auscultation in COVID-19 pneumonia using an electronic stethoscope in isolation wards. To date, little is known about the characteristics of pulmonary auscultation in novel coronavirus (COVID-19) pneumonia. Background: Effective auscultations are often hard to implement in isolation wards.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
